Guidelines for Caregiving for Individuals with Paraplegia and Tetraplegia
- Comprehensive Care for Patients with Spinal Cord Injury (SCI) leading to Paraplegia or Tetraplegia
- Initial Phase Management: Preventing Complications
- Respiratory Management in High Cervical Injuries
- Skin Integrity and Pressure Sore Prevention
- Bowel Management
- Autonomic Dysreflexia Management
- Deep Vein Thrombosis (DVT) and Pulmonary Embolism (PE) Prevention
- Psychological Support and Rehabilitation Planning
- Safe Patient Handling Techniques for Caregivers
- Multidisciplinary Team Approach
- Common Medical Issues in SCI and their Management (Table)
- Long-Term Considerations and Quality of Life
- When to Seek Immediate Medical Attention
- References
Comprehensive Care for Patients with Spinal Cord Injury (SCI) leading to Paraplegia or Tetraplegia
Caring for individuals who have sustained a spinal cord injury (SCI) resulting in paraplegia (paralysis of the lower extremities) or tetraplegia (quadriplegia, paralysis of all four extremities) is a complex and multifaceted endeavor. It requires a comprehensive approach addressing numerous physiological systems to prevent complications, maintain health, and optimize quality of life. These guidelines highlight key areas of focus in caregiving.
Initial Phase Management: Preventing Complications
Urinary Tract Management
During the initial phase of paraplegia or tetraplegia, particularly during spinal shock, preventing urinary tract damage is crucial. The bladder often loses its normal reflex function (neurogenic bladder), leading to urinary retention. The patient may not be able to feel when the bladder is full. This can cause overstretching and damage to the bladder's muscular wall (detrusor muscle), increasing the risk of vesicoureteral reflux, hydronephrosis, and kidney damage. To prevent these complications, urologists or trained healthcare professionals perform bladder drainage. This also helps prevent urinary tract infections (UTIs), which are common in this population.
The most effective method for long-term bladder management is often **intermittent catheterization (IC)**, performed by trained individuals (including the patient if able, or caregivers) at regular intervals. Alternative methods include:
- Indwelling Urethral Catheterization: Using a catheter left in place with a closed drainage system. This carries a higher risk of infection, bladder stones, and urethral trauma in paralyzed patients if used long-term.
- Suprapubic Cystostomy: A catheter inserted directly into the bladder through an incision in the lower abdomen. This may be considered for long-term drainage in some individuals but also carries infection risks.
If the sacral segments of the spinal cord (S2-S4, controlling bladder reflexes) are intact and spinal shock resolves, patients may eventually achieve automatic or reflex bladder emptying. Initially, this might manifest as reflexive urination (incontinence) between catheterizations. Later, patients can sometimes learn techniques to trigger urination (e.g., crede maneuver, tapping over the bladder). However, if significant residual urine volume persists, increasing the risk of bladder infection or damage, further urological procedures or continued intermittent/indwelling catheterization may be necessary.
Cardiovascular Stability
Patients with acute spinal cord injuries, especially those causing spinal shock (a temporary state of suppressed reflex activity below the level of injury), often require cardiovascular therapy to manage hemodynamic instability. This can include:
- Hypotension (Low Blood Pressure): Common, particularly with cervical or high thoracic injuries, due to loss of sympathetic tone. Management may involve intravenous fluids and vasopressor medications.
- Hypertension (High Blood Pressure): Can occur, especially as part of autonomic dysreflexia (see below).
- Bradycardia (Slow Heart Rate): May also occur with high cervical injuries.
Fluid management is crucial to correct imbalances in blood volume and maintain adequate perfusion.
Gastrointestinal Protection
Patients with complete spinal cord injuries, particularly in the acute phase, are at an increased risk of developing stress ulcers in the stomach and intestines due to physiological stress and potential autonomic dysfunction. Prophylactic medications such as H2-receptor antagonists (e.g., cimetidine, ranitidine - though ranitidine has been largely withdrawn from many markets) or proton pump inhibitors (PPIs) are often effective for preventing or treating these gastrointestinal ulcers.
Respiratory Management in High Cervical Injuries
High cervical spinal cord injuries (e.g., above C5, affecting the phrenic nerve which innervates the diaphragm) can cause varying degrees of respiratory failure due to impaired function of the diaphragm and intercostal muscles (muscles between the ribs). This respiratory compromise may necessitate:
- Mechanical Ventilation: In severe cases, particularly with injuries at C3 or above, long-term mechanical ventilation may be required.
- Bronchopulmonary Rehabilitation/Hygiene: Techniques to clear airway secretions, such as assisted coughing, postural drainage, and chest physiotherapy, are vital.
- Respiratory Therapy: For incomplete respiratory failure with a forced vital capacity (FVC) typically between 10-20 ml/kg, respiratory therapy including deep breathing exercises, incentive spirometry, and inhalations (e.g., bronchodilators if needed) along with chest massage (physiotherapy) is recommended.
- Negative Pressure Corset/Ventilation: Historically, a negative pressure corset or cuirass ventilator was sometimes used to assist breathing and help prevent atelectasis (lung collapse) and respiratory muscle fatigue, particularly in patients with SCI below the C5 level who retain some diaphragmatic function.
- Airway Management: In severe respiratory failure or if airway protection is compromised, tracheal intubation (using an endoscope or fiberoptic guidance if the cervical spine is unstable) followed by tracheostomy may be necessary to ensure a secure airway for long-term ventilation and efficient removal of bronchial secretions.
- Diaphragmatic Nerve Electrical Stimulation (Phrenic Nerve Pacing): This is a promising newer method for selected patients with injuries at the C5 level or above who have intact phrenic nerves but paralyzed diaphragms. It involves surgically implanting electrodes to stimulate the phrenic nerves, causing diaphragmatic contraction and enabling breathing without continuous mechanical ventilation.
Skin Integrity and Pressure Sore Prevention
Prolonged immobility dramatically increases the risk of skin breakdown and the development of pressure sores (decubitus ulcers), particularly over bony prominences (sacrum, hips, heels, elbows). This risk is heightened by impaired sensation and compromised circulation below the level of injury. Key preventive measures include:
- Regular Repositioning: Patients should have their position changed frequently (e.g., every 2-3 hours when in bed, more often when seated in a wheelchair) to relieve pressure.
- Skin Care: Keeping the skin clean and dry. Using emollients to maintain skin hydration. Regular skin inspection for early signs of redness or breakdown.
- Specialized Bedding and Seating: Use of pressure-relieving mattresses (e.g., alternating pressure, low air loss) and wheelchair cushions is essential.
- Nutrition and Hydration: Adequate protein and calorie intake, along with good hydration, supports skin health and healing.
Specially designed functional beds that assist with repositioning and help to evenly distribute body weight can significantly reduce pressure on bony prominences and aid in pressure sore prevention.
Bowel Management
Most patients with significant paralysis (paraplegia or tetraplegia) experience neurogenic bowel dysfunction, leading to constipation, fecal incontinence, or difficulty with evacuation. A regular bowel management program is essential to prevent complications such as fecal impaction, bowel obstruction, or autonomic dysreflexia triggered by bowel distension. This program usually involves:
- Scheduled bowel movements (e.g., daily or every other day).
- Dietary fiber and adequate fluid intake.
- Use of stool softeners, suppositories, or mini-enemas as needed.
- Digital stimulation or manual evacuation if necessary.
Patients need to monitor bowel function and ensure regular bowel movements (at least twice weekly is a general guideline, but individual programs vary) to maintain health and comfort.
Autonomic Dysreflexia Management
Patients with spinal cord injuries at or above the T6 level are at risk for autonomic dysreflexia (AD). This is a potentially life-threatening condition characterized by an imbalanced reflex sympathetic discharge in response to noxious (painful or irritating) stimuli below the level of injury. Common triggers include:
- Bladder distension (full bladder, blocked catheter).
- Bowel distension (constipation, impaction).
- Skin irritation (pressure sores, ingrown toenails, tight clothing).
- Surgical manipulation or other painful procedures.
Symptoms of AD include:
- Sudden onset of severe hypertension (high blood pressure).
- Pounding headache.
- Bradycardia (slow heart rate) or sometimes tachycardia.
- Profuse sweating and flushing of the skin above the level of the spinal cord injury.
- Goosebumps, nasal congestion, blurred vision.
The exact neurophysiological cause of these widespread autonomic disorders is not fully understood but involves loss of supraspinal control over sympathetic reflexes below the injury level. Management of AD involves:
- Sitting the patient upright to help lower blood pressure.
- Identifying and removing the noxious stimulus immediately (e.g., empty bladder, check for bowel impaction, loosen tight clothing).
- Administering fast-acting antihypertensive medications if blood pressure remains dangerously high. Beta-blockers are generally avoided due to the risk of unopposed alpha-adrenergic activity and exacerbating bradycardia.
Some patients with SCI, particularly high cervical injuries, may experience acute bradycardia (a significant drop in heart rate) as a result of vagal stimulation during procedures like tracheal suctioning. This can sometimes be prevented by pre-administering small doses of atropine (an anticholinergic agent).
Deep Vein Thrombosis (DVT) and Pulmonary Embolism (PE) Prevention
Prolonged immobility significantly increases the risk of developing deep vein thrombosis (blood clots in the legs) and subsequent pulmonary embolism (clots traveling to the lungs), which can be life-threatening. PE is a serious early complication, occurring in approximately 30% of patients with paralysis following acute SCI if no prophylaxis is given. Preventive measures include:
- Anticoagulant medications (e.g., low-molecular-weight heparin).
- Graduated compression stockings.
- Intermittent pneumatic compression devices on the legs.
- Early mobilization and range-of-motion exercises as tolerated.
Other risk factors for DVT/PE in this population include skin breakdown over pressure points leading to local inflammation, urinary tract infections (sepsis), and autonomic instability contributing to venous stasis.
Neurotrophic pressure sores are a severe consequence of impaired nerve function (innervation) and prolonged immobility that can follow a spinal compression fracture or other injury leading to spinal cord compression.
Psychological Support and Rehabilitation Planning
Once the patient's acute medical condition stabilizes, psychological support for both the patient and their family, along with comprehensive rehabilitation planning, becomes essential. Spinal cord injury is a life-altering event with significant emotional and psychological impact. Intensive, multidisciplinary rehabilitation programs (involving physiatrists, physical therapists, occupational therapists, psychologists, social workers, and vocational counselors) often yield positive outcomes, particularly for young and middle-aged patients. These programs aim to maximize functional independence, facilitate adaptation to disability, and enable patients to return home and resume meaningful daily lives and community participation.
Patients with lower extremity paralysis (paraplegia) can often perform many self-care procedures with appropriate training and adaptive equipment, sometimes with minimal assistance. Tetraplegic patients require more extensive assistance depending on their level of injury.
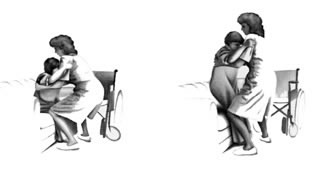
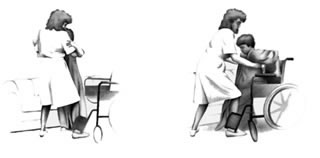
Safe Patient Handling Techniques for Caregivers
Caregivers play a vital role and must use proper body mechanics to prevent injury to themselves while assisting individuals with paralysis. Key principles include:
- Bend Knees, Not Back: Always bend at the knees and hips, keeping the back straight, when lifting or repositioning. Use leg muscles rather than back muscles.
- Keep Load Close: Hold the person or object close to your body.
- Wide Base of Support: Keep feet shoulder-width apart.
- Avoid Twisting: Pivot with your feet instead of twisting your spine.
- Use Assistive Devices: Utilize Hoyer lifts, slide sheets, or transfer boards when appropriate.
- Ask for Help: If a transfer or task is too difficult for one person, get assistance.
Multidisciplinary Team Approach
For detailed information on specific physiotherapy techniques, comprehensive rehabilitation programs, and the use of orthopedic devices or assistive technology for individuals with severe spinal cord conditions and paralysis, it is essential to consult the patient's primary physician and a multidisciplinary team of specialists. This team often includes a neurosurgeon (especially for initial stabilization of spinal trauma, if indicated), a urologist (for bladder management), a rehabilitation specialist (physiatrist), physical therapists, occupational therapists, and other allied health professionals. Spinal orthopedic stabilization in cases of spinal trauma is performed only when clinically necessary to prevent further injury or promote healing.
Common Medical Issues in SCI and their Management (Table)
| Issue/Complication | Common Symptoms/Signs | Key Management/Caregiving Strategies |
|---|---|---|
| Neurogenic Bladder | Urinary retention, incontinence, frequent UTIs, kidney damage risk. | Intermittent catheterization, indwelling/suprapubic catheter, bladder medications, regular urological follow-up. |
| Neurogenic Bowel | Constipation, fecal incontinence, impaction, bowel obstruction risk. | Regular bowel program (diet, fluids, suppositories, digital stimulation), monitor bowel movements. |
| Pressure Sores (Decubitus Ulcers) | Redness, skin breakdown over bony prominences (sacrum, hips, heels). | Regular repositioning (every 2-3 hrs in bed), pressure-relieving surfaces, skin inspection/care, nutrition. |
| Autonomic Dysreflexia (AD) (SCI at T6 or above) | Sudden severe hypertension, pounding headache, bradycardia, sweating/flushing above injury level. | Sit patient upright, identify and remove noxious stimulus (e.g., empty bladder/bowel, check skin), monitor BP, antihypertensives if needed. Emergency. |
| Spasticity | Increased muscle tone, spasms, clonus, contracture risk. | Stretching, range-of-motion exercises, positioning, anti-spasticity medications (baclofen, tizanidine), botulinum toxin injections. |
| Deep Vein Thrombosis (DVT) / Pulmonary Embolism (PE) | Leg swelling, pain, warmth (DVT); shortness of breath, chest pain, tachycardia (PE). Often asymptomatic. | Prophylactic anticoagulants, compression stockings, pneumatic compression devices, early mobilization if possible. |
| Respiratory Compromise (High SCI) | Weak cough, shortness of breath, recurrent pneumonia, atelectasis. | Assisted coughing, chest physiotherapy, respiratory muscle training, mechanical ventilation/tracheostomy if severe, phrenic nerve pacing. |
| Chronic Pain (Neuropathic/Musculoskeletal) | Burning, shooting, aching pain at or below injury level, or musculoskeletal pain from overuse of upper limbs. | Medications (gabapentinoids, antidepressants, NSAIDs), physical modalities, psychological support, pain specialist consultation. |
Long-Term Considerations and Quality of Life
Long-term care for individuals with paraplegia or tetraplegia focuses on maintaining health, preventing secondary complications, maximizing independence, and promoting a high quality of life. This involves ongoing medical supervision, regular health screenings, access to appropriate therapies and assistive technologies, and support for social, emotional, and vocational reintegration. Advances in medical care and rehabilitation have significantly improved the life expectancy and quality of life for many individuals living with spinal cord injuries.
When to Seek Immediate Medical Attention
Caregivers and individuals with SCI should be vigilant for signs that require immediate medical attention, including but not limited to:
- Symptoms of Autonomic Dysreflexia (severe headache, very high blood pressure).
- Signs of severe infection (high fever, chills, worsening lethargy), especially urinary tract or respiratory infections, or infected pressure sores.
- Sudden onset or worsening of respiratory distress.
- Signs of DVT (unilateral leg swelling, pain, warmth) or PE (sudden shortness of breath, chest pain).
- Significant changes in neurological status (e.g., new weakness, loss of sensation).
- Uncontrolled pain.
- Blocked urinary catheter or inability to pass urine.
- Severe constipation or signs of bowel obstruction.
- New or worsening skin breakdown.
Prompt medical intervention is crucial in managing these acute issues and preventing further complications.
References
- Consortium for Spinal Cord Medicine. Bladder management for adults with spinal cord injury: a clinical practice guideline for health-care providers. J Spinal Cord Med. 2006;29(5):527-73.
- Consortium for Spinal Cord Medicine. Pressure ulcer prevention and treatment following spinal cord injury: a clinical practice guideline for health-care professionals. 2nd ed. Paralyzed Veterans of America; 2014.
- Krassioukov A, Warburton DE, Teasell R, Eng JJ; Spinal Cord Injury Rehabilitation Evidence Research Team. A systematic review of the management of autonomic dysreflexia after spinal cord injury. Arch Phys Med Rehabil. 2009 Apr;90(4):682-95.
- McKinley WO, Gittler MS, Kirshblum SC, et al. Spinal cord injury medicine. 1. Medical complications after spinal cord injury: identification and management. Arch Phys Med Rehabil. 2002 Mar;83(3 Suppl 1):S58-64, S90-8.
- National Institute of Neurological Disorders and Stroke (NINDS). Spinal Cord Injury: Hope Through Research. NIH Publication No. 13-160. Accessed [Current Date].
- Teasell RW, Arnold JM, Krassioukov A, Delaney GA. Cardiovascular consequences of_spinal_cord_injury: Pathophysiology, diagnosis, and management. Arch Phys Med Rehabil. 2000 Apr;81(4):523-31.
- Consortium for Spinal Cord Medicine. Preservation of upper limb function following spinal cord injury: a clinical practice guideline for health-care professionals. Paralyzed Veterans of America; 2005.
- Cardenas DD, Hooton TM. Urinary tract infections in persons with spinal cord injury. Arch Phys Med Rehabil. 1995 Mar;76(3):272-80.
See also
- Anatomy of the spine
- Ankylosing spondylitis (Bechterew's disease)
- Back pain by the region of the spine:
- Back pain during pregnancy
- Coccygodynia (tailbone pain)
- Compression fracture of the spine
- Dislocation and subluxation of the vertebrae
- Herniated and bulging intervertebral disc
- Lumbago (low back pain) and sciatica
- Osteoarthritis of the sacroiliac joint
- Osteocondritis of the spine
- Osteoporosis of the spine
- Guidelines for Caregiving for Individuals with Paraplegia and Tetraplegia
- Sacrodinia (pain in the sacrum)
- Sacroiliitis (inflammation of the sacroiliac joint)
- Scheuermann-Mau disease (juvenile osteochondrosis)
- Scoliosis, poor posture
- Spinal bacterial (purulent) epiduritis
- Spinal cord diseases:
- Spinal spondylosis
- Spinal stenosis
- Spine abnormalities
- Spondylitis (osteomyelitic, tuberculous)
- Spondyloarthrosis (facet joint osteoarthritis)
- Spondylolisthesis (displacement and instability of the spine)
- Symptom of pain in the neck, head, and arm
- Pain in the thoracic spine, intercostal neuralgia
- Vertebral hemangiomas (spinal angiomas)
- Whiplash neck injury, cervico-cranial syndrome