Spinal shock after severe spinal cord injury
Spinal shock after severe spinal cord injury
After severe spinal cord injury, generalised flaccidity below the level of the lesion supervenes, but it is rare for all reflexes to be absent in the first few weeks except in lower motor neurone lesions. The classical description of spinal shock as the period following injury during which all spinal reflexes are absent should therefore be discarded, particularly as almost a third of patients examined within 1–3 hours of injury have reflexes present.
The delayed plantar response (DPR) is present in all patients with complete injuries. It is demonstrated by pressing firmly with a blunt instrument from the heel toward the toes along the lateral sole of the foot and continuing medially across the volar aspect of the metatarsal heads. Following the stimulus the toes flex and relax in delayed sequence. The flexion component can be misinterpreted as a normal plantar response.
The deep tendon reflexes are more predictable: usually absent in complete cord lesions, and present in the majority of patients with incomplete injuries.
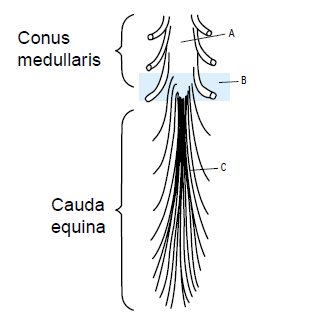
The anal and bulbocavernosus reflexes both depend on intact sacral reflex arcs. The anal reflex is an externally visible contraction of the anal sphincter in response to perianal pin prick. The bulbocavernosus reflex is a similar contraction of the anal sphincter felt with the examining finger in response to squeezing the glans penis. They may aid in distinguishing between an upper motor neurone lesion, in which the reflex may not return for several days, and a lower motor neurone lesion, in which the reflex remains ablated unless neurological recovery occurs. Examples of such lower motor neurone lesions are injuries to the conus and cauda equina.
See also
- At the accident:
- History and epidemiology of spinal cord injury
- Spinal injuries management at the scene of the accident
- Evacuation and initial management at hospital:
- Evacuation and transfer to hospital of patients with spinal cord injuries
- Initial management of patients with spinal cord injuries at the receiving hospital
- Neurological assessment of patients with spinal cord injuries
- Spinal shock after severe spinal cord injury
- Partial spinal cord injury syndromes
- Radiological investigations:
- Initial radiography of patients with spinal cord injuries
- Cervical injuries
- Thoracic and lumbar injuries
- Early management and complications of spinal cord injuries — I:
- Respiratory complications
- Cardiovascular complications
- Prophylaxis against thromboembolism
- Initial bladder management
- The gastrointestinal tract
- Use of steroids and antibiotics
- The skin and pressure areas
- Care of the joints and limbs
- Later analgesia
- Trauma re-evaluation
- Early management and complications of spinal cord injuries — II:
- The anatomy of spinal cord injury
- The spinal injury (cervical, thoracic and lumbar spine)
- Transfer to a spinal injuries unit
- Medical management in the spinal injuries unit:
- The cervical spine injuries
- The cervicothoracic junction injuries
- Thoracic injuries
- Thoracolumbar and lumbar injuries
- Deep vein thrombosis and pulmonary embolism
- Autonomic dysreflexia
- Biochemical disturbances
- Para-articular heterotopic ossification
- Spasticity
- Contractures
- Pressure sores
- Urological management of patients with spinal cord injury:
- Nursing for people with spinal cord lesion:
- Physiotherapy after spinal cord injury:
- Respiratory management
- Mobilisation into a wheelchair
- Rehabilitation
- Recreation
- Incomplete lesions
- Children
- Occupational therapy after spinal cord injury:
- Hand and upper limb management
- Home resettlement
- Activities of daily living
- Communication
- Mobility
- Leisure
- Work
- Social needs of patient and family:
- Transfer of care from hospital to community:
- Education of patients
- Teaching the family and community staff
- Preparation for discharge from hospital
- Easing transfer from hospital to community
- Travel and holidays
- Follow-up
- Later management and complications after spinal cord injury — I:
- Late spinal instability and spinal deformity
- Pathological fractures
- Post-traumatic syringomyelia (syrinx, cystic myelopathy)
- Pain
- Sexual function
- Later management and complications after spinal cord injury — II:
- Later respiratory management of high tetraplegia
- Psychological factors
- The hand in tetraplegia
- Functional electrical stimulation
- Ageing with spinal cord injury
- Prognosis
- Spinal cord injury in the developing world: