Neurological assessment of patients with spinal cord injuries
Neurological assessment of patients with spinal cord injuries
In spinal cord injury the neurological examination must include assessment of the following:
- Sensation to pin prick (spinothalamic tracts)
- Sensation to fine touch and joint position sense (posterior columns)
- Power of muscle groups according to the Medical Research Council scale (corticospinal tracts)
- Reflexes (including abdominal, anal, and bulbocavernosus)
- Cranial nerve function (may be affected by high cervical injury, e.g. dysphagia)
By examining the dermatomes and myotomes in this way, the level and completeness of the spinal cord injury and the presence of other neurological damage such as brachial plexus injury are assessed. The last segment of normal spinal cord function, as judged by clinical examination, is referred to as the neurological level of the lesion. This does not necessarily correspond with the level of bony injury (Figure 5.1), so the neurological and bony diagnoses should both be recorded. Sensory or motor sparing may be present below the injury.
Traditionally, incomplete spinal cord lesions have been defined as those in which some sensory or motor function is preserved below the level of neurological injury. The American Spinal Injury Association (ASIA) has now produced the ASIA impairment scale modified from the Frankel grades (see page 74). Incomplete injuries have been redefined as those associated with some preservation of sensory or motor function below the neurological level, including the lowest sacral segment. This is determined by the presence of sensation both superficially at the mucocutaneous junction and deeply within the anal canal, or alternatively by intact voluntary contraction of the external anal sphincter on digital examination. ASIA also describes the zone of partial preservation (ZPP) which refers to the dermatomes and myotomes that remain partially innervated below the main neurological level. The exact number of segments so affected should be recorded for both sides of the body. The term ZPP is used only with injuries that do not satisfy the ASIA definition of “incomplete”.
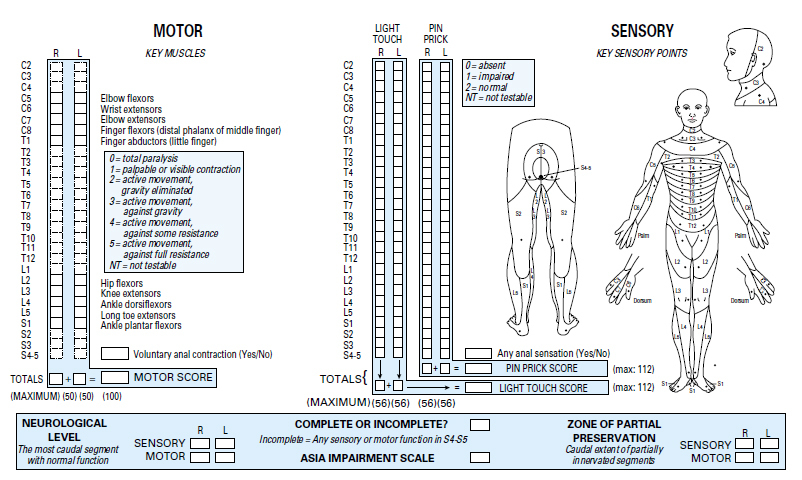
ASIA has produced a form incorporating these definitions (Figure 2.8). The muscles tested by ASIA are chosen because of the consistency of their nerve supply by the segments indicated, and because they can all be tested with the patient in the supine position.
ASIA also states that other muscles should be evaluated, but their grades are not used in determining the motor score and level. The muscles not listed on the ASIA Standard Neurological Classification form, with their nerve supply, are as follows:
- Diaphragm — C3,4,5
- Shoulder abductors — C5
- Supinators/pronators — C6
- Wrist flexors — C7
- Finger extensors — C7
- Intrinsic hand muscles — T1
- Hip adductors — L2,3
- Knee flexors — L4,5 S1
- Toe flexors — S1,2
Reflexes and their nerve supply |
|
| Biceps jerk | C5,6 |
| Supinator jerk | C6 |
| Triceps jerk | C7 |
| Abdominal reflex | T8–12 |
| Knee jerk | L3,4 |
| Ankle jerk | L5,S1 |
| Bulbocavernosus reflex | S3,4 |
| Anal reflex | S5 |
| Plantar reflex | L5,S1 |
Spinal reflexes after cord injury
![]() Note: Almost one third of patients with spinal cord injury examined within 1–3 hours of injury have reflexes
Note: Almost one third of patients with spinal cord injury examined within 1–3 hours of injury have reflexes
Plantar reflex after cord injury
Distinguish between:
- Delayed plantar response — present in all complete injuries
- Normal plantar response
ASIA Impairment Scale—used in grading the degree of impairment:
- A = Complete. No sensory or motor function is preserved in the sacral segments S4–S5
- B = Incomplete. Sensory but not motor function is preserved below the neurological level and extends through the sacral segments S4–S5
- C = Incomplete. Motor function is preserved below the neurological level, and the majority of key muscles below the neurological level have a muscle grade less than 3
- D = Incomplete. Motor function is preserved below the neurological level, and the majority of key muscles below the neurological level have a muscle grade greater than or equal to 3
- E = Normal. Sensory and motor function is normal
See also
- At the accident:
- History and epidemiology of spinal cord injury
- Spinal injuries management at the scene of the accident
- Evacuation and initial management at hospital:
- Evacuation and transfer to hospital of patients with spinal cord injuries
- Initial management of patients with spinal cord injuries at the receiving hospital
- Neurological assessment of patients with spinal cord injuries
- Spinal shock after severe spinal cord injury
- Partial spinal cord injury syndromes
- Radiological investigations:
- Initial radiography of patients with spinal cord injuries
- Cervical injuries
- Thoracic and lumbar injuries
- Early management and complications of spinal cord injuries — I:
- Respiratory complications
- Cardiovascular complications
- Prophylaxis against thromboembolism
- Initial bladder management
- The gastrointestinal tract
- Use of steroids and antibiotics
- The skin and pressure areas
- Care of the joints and limbs
- Later analgesia
- Trauma re-evaluation
- Early management and complications of spinal cord injuries — II:
- The anatomy of spinal cord injury
- The spinal injury (cervical, thoracic and lumbar spine)
- Transfer to a spinal injuries unit
- Medical management in the spinal injuries unit:
- The cervical spine injuries
- The cervicothoracic junction injuries
- Thoracic injuries
- Thoracolumbar and lumbar injuries
- Deep vein thrombosis and pulmonary embolism
- Autonomic dysreflexia
- Biochemical disturbances
- Para-articular heterotopic ossification
- Spasticity
- Contractures
- Pressure sores
- Urological management of patients with spinal cord injury:
- Nursing for people with spinal cord lesion:
- Physiotherapy after spinal cord injury:
- Respiratory management
- Mobilisation into a wheelchair
- Rehabilitation
- Recreation
- Incomplete lesions
- Children
- Occupational therapy after spinal cord injury:
- Hand and upper limb management
- Home resettlement
- Activities of daily living
- Communication
- Mobility
- Leisure
- Work
- Social needs of patient and family:
- Transfer of care from hospital to community:
- Education of patients
- Teaching the family and community staff
- Preparation for discharge from hospital
- Easing transfer from hospital to community
- Travel and holidays
- Follow-up
- Later management and complications after spinal cord injury — I:
- Late spinal instability and spinal deformity
- Pathological fractures
- Post-traumatic syringomyelia (syrinx, cystic myelopathy)
- Pain
- Sexual function
- Later management and complications after spinal cord injury — II:
- Later respiratory management of high tetraplegia
- Psychological factors
- The hand in tetraplegia
- Functional electrical stimulation
- Ageing with spinal cord injury
- Prognosis
- Spinal cord injury in the developing world: