Initial management of patients with spinal cord injuries at the receiving hospital
Primary survey
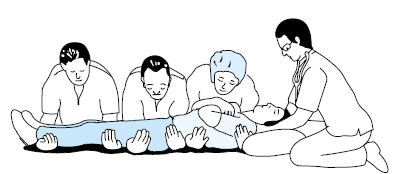
When the patient arrives at the nearest major emergency department, a detailed history must be obtained from ambulance staff, witnesses, and if possible the patient. Simultaneously, the patient is transferred to the trauma trolley and this must be expeditious but smooth. If the patient is attached to a spinal board, this is an ideal transfer device and resuscitation can continue on the spinal board with only momentary interruption. Alternatively a scoop stretcher can be used for the transfer but this will take longer. In the absence of either device, the patient can be subjected to a coordinated spinal lift but this requires training.
A full general and neurological assessment must be undertaken in accordance with the principles of advanced trauma life support (ATLS). The examination must be thorough because spinal trauma is frequently associated with multiple injuries. As always, the patient’s airway, breathing and circulation (“ABC”— in that order) are the first priorities in resuscitation from trauma. If not already secure, the cervical spine is immobilised in the neutral position as the airway is assessed. Following attention to the ABC, a central nervous system assessment is undertaken and any clothing is removed. This sequence constitutes the primary survey of ATLS. The spinal injury itself can directly affect the airway (for example by producing a retropharyngeal haematoma or tracheal deviation) as well as the respiratory and circulatory systems (see chapter 4).
Associated injuries — new injury admissions to Duke of Cornwall Spinal Treatment Centre 1997–99:
Spinal cord injury is accompanied by: |
% |
| Head injuries (coma of more than 6 hours’ duration, brain contusion or skull fracture) | in 12% |
| Chest injuries (requiring active treatment, or rib fractures) | in 19% |
| Abdominal injuries (requiring laparotomy) | in 3% |
| Limb injuries | in 20% |
Secondary survey
Once the immediately life-threatening injuries have been addressed, the secondary (head to toe) survey that follows allows other serious injuries to be identified. Areas that are not being examined should be covered and kept warm, and body temperature should be monitored. In the supine position, the cervical and lumbar lordoses may be palpated by sliding a hand under the patient. A more comprehensive examination is made during the log roll. Unless there is an urgent need to inspect the back, the log roll is normally undertaken near the end of the secondary survey by a team of four led by the person who holds the patient’s head. If neurological symptoms or signs are present, a senior doctor should be present and a partial roll to about 45˚ may be sufficient. A doctor who is not involved with the log roll must examine the back for specific signs of injury including local bruising or deformity of the spine (e.g. a gibbus or an increased interspinous gap) and vertebral tenderness. The whole length of the spine must be palpated, as about 10% of patients with an unstable spinal injury have another spinal injury at a different level. Priapism and diaphragmatic breathing invariably indicate a high spinal cord lesion. The presence of warm and well-perfused peripheries in a hypotensive patient should always raise the possibility of neurogenic shock attributable to spinal cord injury in the differential diagnosis. At the end of the secondary survey, examination of the peripheral nervous system must not be neglected.
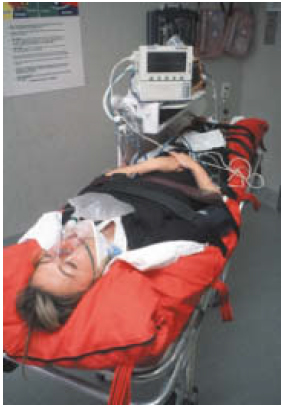
The log roll during the secondary survey provides an ideal opportunity to remove the spinal board from the patient. It has been demonstrated that high pressure exists at the interfaces between the board and the occiput, scapulae, sacrum, and heels. It is generally recommended that the spinal board is removed within 30 minutes of its application whenever possible. The head and neck can then be splinted to the trauma trolley. If full splintage is required following removal of the spinal board, especially for transit between hospitals, use of a vacuum mattress is recommended. This device is contoured to the patient before air is evacuated from it with a pump. The vacuum causes the plastic beads within the mattress to lock into position. Interface pressures are much lower when a vacuum mattress is used and patients find the device much more comfortable than a spinal board. Paediatric vacuum mattresses are also available and they may be used at the accident scene.
Diagnosis of intra-abdominal trauma often difficult because of:
- impaired or absent abdominal sensation
- absent abdominal guarding or rigidity, because of flaccid paralysis
- paralytic ileus
If blunt abdominal trauma suspected:
- peritoneal lavage
- abdominal CT scan with contrast
A specific clinical problem in spinal cord injury is the early diagnosis of intra-abdominal trauma during the secondary survey. This may be very difficult in patients with high cord lesions (above the seventh thoracic segment) during the initial phase of spinal shock, when paralytic ileus and abdominal distension are usual. Abdominal sensation is impaired, and this, together with the flaccid paralysis, means that the classical features of an intra-abdominal emergency may be absent. The signs of peritoneal irritation do not develop but pain may be referred to the shoulder from the diaphragm and this is an important symptom. When blunt abdominal trauma is suspected, peritoneal lavage or computed tomography is recommended unless clinical concern justifies immediate laparotomy. Abdominal bruising from seat belts, especially isolated lap belts in children, is associated with injuries to the bowel, pancreas and lumbar spine.
See also
- At the accident:
- History and epidemiology of spinal cord injury
- Spinal injuries management at the scene of the accident
- Evacuation and initial management at hospital:
- Evacuation and transfer to hospital of patients with spinal cord injuries
- Initial management of patients with spinal cord injuries at the receiving hospital
- Neurological assessment of patients with spinal cord injuries
- Spinal shock after severe spinal cord injury
- Partial spinal cord injury syndromes
- Radiological investigations:
- Initial radiography of patients with spinal cord injuries
- Cervical injuries
- Thoracic and lumbar injuries
- Early management and complications of spinal cord injuries — I:
- Respiratory complications
- Cardiovascular complications
- Prophylaxis against thromboembolism
- Initial bladder management
- The gastrointestinal tract
- Use of steroids and antibiotics
- The skin and pressure areas
- Care of the joints and limbs
- Later analgesia
- Trauma re-evaluation
- Early management and complications of spinal cord injuries — II:
- The anatomy of spinal cord injury
- The spinal injury (cervical, thoracic and lumbar spine)
- Transfer to a spinal injuries unit
- Medical management in the spinal injuries unit:
- The cervical spine injuries
- The cervicothoracic junction injuries
- Thoracic injuries
- Thoracolumbar and lumbar injuries
- Deep vein thrombosis and pulmonary embolism
- Autonomic dysreflexia
- Biochemical disturbances
- Para-articular heterotopic ossification
- Spasticity
- Contractures
- Pressure sores
- Urological management of patients with spinal cord injury:
- Nursing for people with spinal cord lesion:
- Physiotherapy after spinal cord injury:
- Respiratory management
- Mobilisation into a wheelchair
- Rehabilitation
- Recreation
- Incomplete lesions
- Children
- Occupational therapy after spinal cord injury:
- Hand and upper limb management
- Home resettlement
- Activities of daily living
- Communication
- Mobility
- Leisure
- Work
- Social needs of patient and family:
- Transfer of care from hospital to community:
- Education of patients
- Teaching the family and community staff
- Preparation for discharge from hospital
- Easing transfer from hospital to community
- Travel and holidays
- Follow-up
- Later management and complications after spinal cord injury — I:
- Late spinal instability and spinal deformity
- Pathological fractures
- Post-traumatic syringomyelia (syrinx, cystic myelopathy)
- Pain
- Sexual function
- Later management and complications after spinal cord injury — II:
- Later respiratory management of high tetraplegia
- Psychological factors
- The hand in tetraplegia
- Functional electrical stimulation
- Ageing with spinal cord injury
- Prognosis
- Spinal cord injury in the developing world: