Xalatan Drug Description: Detailed Datasheet
- Generic Name: latanoprost ophthalmic
- Brand Name: Xalatan
- Drug Class: Antiglaucoma, Prostaglandin Agonists
side effects drug center xalatan (latanoprost ophthalmic) drug
- Related Drugs
- Health Resources
- Related Supplements
- Xalatan User Reviews
Drug Description
XALATAN®
(latanoprost) Ophthalmic Solution/p>
DESCRIPTION
Latanoprost is a prostaglandin F2α analogue. Its chemical name is isopropyl-(Z)-7[(1R,2R,3R,5S)3,5dihydroxy-2-[(3R)-3-hydroxy-5-phenylpentyl]cyclopentyl]-5-heptenoate. Its molecular formula is C26H40O5 and its chemical structure is:
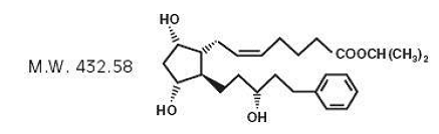 |
Latanoprost is a colorless to slightly yellow oil that is very soluble in acetonitrile and freely soluble in acetone, ethanol, ethyl acetate, isopropanol, methanol, and octanol. It is practically insoluble in water.
XALATAN (latanoprost ophthalmic solution) 0.005% is supplied as a sterile, isotonic, buffered aqueous solution of latanoprost with a pH of approximately 6.7 and an osmolality of approximately 267 mOsmol/kg. Each mL of XALATAN contains 50 mcg of latanoprost. Benzalkonium chloride, 0.02% is added as a preservative. The inactive ingredients are: sodium chloride, sodium dihydrogen phosphate monohydrate, disodium hydrogen phosphate anhydrous, and water for injection. One drop contains approximately 1.5 mcg of latanoprost.
Indications & Dosage
INDICATIONS
XALATAN is indicated for the reduction of elevated intraocular pressure in patients with open-angle glaucoma or ocular hypertension.
DOSAGE AND ADMINISTRATION
The recommended dosage is one drop in the affected eye(s) once daily in the evening. If one dose is missed, treatment should continue with the next dose as normal.
The dosage of XALATAN should not exceed once daily; the combined use of two or more prostaglandins, or prostaglandin analogs including XALATAN is not recommended. It has been shown that administration of these prostaglandin drug products more than once daily may decrease the intraocular pressure (IOP) lowering effect or cause paradoxical elevations in IOP.
Reduction of the IOP starts approximately 3 to 4 hours after administration and the maximum effect is reached after 8 to 12 hours.
XALATAN may be used concomitantly with other topical ophthalmic drug products to lower IOP. If more than one topical ophthalmic drug is being used, the drugs should be administered at least five (5) minutes apart. Contact lenses should be removed prior to the administration of XALATAN, and may be reinserted 15 minutes after administration
HOW SUPPLIED
Dosage Forms And Strengths
Sterile ophthalmic solution containing 50 mcg/mL latanoprost.
Storage And Handling
XALATAN is a clear, isotonic, buffered, preserved colorless solution of latanoprost 0.005% (50 mcg/mL). It is supplied as a 2.5 mL solution in a 5 mL clear low density polyethylene bottle with a clear polyethylene dropper tip, a turquoise high density polyethylene screw cap, and a tamper-evident clear low density polyethylene overcap.
2.5 mL fill, 0.005% (50 mcg/mL): Package of 1 bottle: NDC
0013-8303-04
2.5 mL fill, 0.005% (50 mcg/mL): Multi-pack of 3 bottles: NDC 0013-8303-01
Storage
Protect from light. Store unopened bottle(s) under refrigeration at 2° to 8°C (36° to 46°F). During shipment to the patient, the bottle may be maintained at temperatures up to 40°C (104°F) for a period not exceeding 8 days. Once a bottle is opened for use, it may be stored at room temperature up to 25°C (77°F) for 6 weeks.
Distributed by: Pharmacia & Upjohn Co., Division of Pfizer Inc., NY, NY 10017. Pfizer Manufacturing Belgium NV Puurs, Belgium. Revised: n/a
Side Effects & Drug Interactions
SIDE EFFECTS
The following adverse reactions were reported in postmarketing experience and are discussed in greater detail in other sections of the label:
- Iris pigmentation changes [see WARNINGS AND PRECAUTIONS]
- Eyelid skin darkening [see WARNINGS AND PRECAUTIONS]
- Eyelash changes (increased length, thickness, pigmentation, and number of lashes) [see WARNINGS AND PRECAUTIONS]
- Intraocular inflammation (iritis/uveitis) [see WARNINGS AND PRECAUTIONS]
- Macular edema, including cystoid macular edema [see WARNINGS AND PRECAUTIONS]
Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, the adverse reaction rates observed in the clinical studies of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in clinical practice.
XALATAN was studied in three multicenter, randomized, controlled clinical trials. Patients received 50 mcg/mL XALATAN once daily or 5 mg/mL active-comparator (timolol) twice daily. The patient population studied had a mean age of 65±10 years. Seven percent of patients withdrew before the 6-month endpoint.
Table 1: Ocular Adverse Reactions and Ocular
Signs/Symptoms Reported by 5-15% of Patients Receiving Latanoprost
| Symptom/Finding | Adverse Reactions (incidence (%)) | |
| Latanoprost (n=460) |
Timolol (n=369) |
|
| Foreign body sensation | 13 | 8 |
| Punctate keratitis | 10 | 9 |
| Stinging | 9 | 12 |
| Conjunctival hyperemia | 8 | 3 |
| Blurred vision | 8 | 8 |
| Itching | 8 | 8 |
| Burning | 7 | 8 |
| Increased pigmentation of the Iris | 7 | 0 |
Less than 1% of the patients treated with XALATAN required discontinuation of therapy because of intolerance to conjunctival hyperemia.
Table 2: Adverse Reactions
That Were Reported in 1-5% of Patients Receiving Latanoprost
| Adverse Reactions (incidence (%)) | ||
| Latanoprost (n=460) |
Timolol (n=369) |
|
| Ocular Events/Signs and Symptoms | ||
| Excessive tearing | 4 | 6 |
| Eyelid discomfort/pain | 4 | 2 |
| Dry eye | 3 | 3 |
| Eye pain | 3 | 3 |
| Eyelid margin crusting | 3 | 3 |
| Erythema of the eyelid | 3 | 2 |
| Photophobia | 2 | 1 |
| Eyelid edema | 1 | 3 |
| Systemic Events | ||
| Upper respiratory tract infection/nasopharyngitis/influenza | 3 | 3 |
| Myalgia/arthralgia/back pain | 1 | 0.5 |
| Rash/allergic skin reaction | 1 | 0.3 |
The ocular event/signs and symptoms of blepharitis have been identified as “commonly observed” through analysis of clinical trial data.
Postmarketing Experience
The following reactions have been identified during postmarketing use of XALATAN in clinical practice. Because they are reported voluntarily from a population of unknown size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure. The reactions, which have been chosen for inclusion due to either their seriousness, frequency of reporting, possible causal connection to XALATAN, or a combination of these factors, include:
Nervous System disorders: Dizziness; headache; toxic epidermal necrolysis
Eye Disorders: Eyelash and vellus hair changes of the eyelid (increased length, thickness, pigmentation, and number of eyelashes); keratitis; corneal edema and erosions; intraocular inflammation (iritis/uveitis); macular edema, including cystoid macular edema; trichiasis; periorbital and lid changes resulting in deepening of the eyelid sulcus; iris cyst; eyelid skin darkening; localised skin reaction on the eyelids; conjunctivitis; pseudopemphigoid of the ocular conjunctiva
Respiratory, Thoracic and Mediastinal Disorders: Asthma and exacerbation of asthma; dyspnea
Skin and Subcutaneous Tissue Disorders: Pruritus
Infections and Infestations: Herpes keratitis
Cardiac Disorders: Angina; palpitations; angina unstable
General Disorders and Administration Site Conditions: Chest pain
DRUG INTERACTIONS
In vitro studies have shown that precipitation occurs when eye drops containing thimerosal are mixed with XALATAN. If such drugs are used, they should be administered at least five (5) minutes apart.
The combined use of two or more prostaglandins, or prostaglandin analogs including XALATAN is not recommended. It has been shown that administration of these prostaglandin drug products more than once daily may decrease the IOP lowering effect or cause paradoxical elevations in IOP.
Warnings & Precautions
WARNINGS
Included as part of the PRECAUTIONS section.
PRECAUTIONS
Pigmentation
XALATAN has been reported to cause changes to pigmented tissues. The most frequently reported changes have been increased pigmentation of the iris, periorbital tissue (eyelid), and eyelashes. Pigmentation is expected to increase as long as latanoprost is administered.
The pigmentation change is due to increased melanin content in the melanocytes rather than to an increase in the number of melanocytes. After discontinuation of latanoprost, pigmentation of the iris is likely to be permanent, while pigmentation of the periorbital tissue and eyelash changes have been reported to be reversible in some patients. Patients who receive treatment should be informed of the possibility of increased pigmentation. Beyond 5 years the effects of increased pigmentation are not known [see Clinical Studies].
Iris color change may not be noticeable for several months to years. Typically, the brown pigmentation around the pupil spreads concentrically towards the periphery of the iris and the entire iris or parts of the iris become more brownish. Neither nevi nor freckles of the iris appear to be affected by treatment. While treatment with XALATAN can be continued in patients who develop noticeably increased iris pigmentation, these patients should be examined regularly [see PATIENT INFORMATION].
Eyelash Changes
XALATAN may gradually change eyelashes and vellus hair in the treated eye; these changes include increased length, thickness, pigmentation, the number of lashes or hairs, and misdirected growth of eyelashes. Eyelash changes are usually reversible upon discontinuation of treatment [see PATIENT INFORMATION].
Intraocular Inflammation
XALATAN should be used with caution in patients with a history of intraocular inflammation (iritis/uveitis) and should generally not be used in patients with active intraocular inflammation because inflammation may be exacerbated.
Macular Edema
Macular edema, including cystoid macular edema, has been reported during treatment with XALATAN. XALATAN should be used with caution in aphakic patients, in pseudophakic patients with a torn posterior lens capsule, or in patients with known risk factors for macular edema.
Herpetic Keratitis
Reactivation of Herpes Simplex keratitis has been reported during treatment with XALATAN. XALATAN should be used with caution in patients with a history of herpetic keratitis. XALATAN should be avoided in cases of active herpes simplex keratitis because inflammation may be exacerbated.
Bacterial Keratitis
There have been reports of bacterial keratitis associated with the use of multiple-dose containers of topical ophthalmic products. These containers had been inadvertently contaminated by patients who, in most cases, had a concurrent corneal disease or a disruption of the ocular epithelial surface [see PATIENT INFORMATION].
Use With Contact Lenses
Contact lenses should be removed prior to the administration of XALATAN, and may be reinserted 15 minutes after administration.
Nonclinical Toxicology
Carcinogenesis, Mutagenesis, Impairment Of Fertility
Latanoprost was not carcinogenic in either mice or rats when administered by oral gavage at doses of up to 170 mcg/kg/day (approximately 2800 times the recommended maximum human dose) for up to 20 and 24 months, respectively.
Latanoprost was not mutagenic in bacteria, in mouse lymphoma, or in mouse micronucleus tests. Chromosome aberrations were observed in vitro with human lymphocytes. Additional in vitro and in vivo studies on unscheduled DNA synthesis in rats were negative.
Latanoprost has not been found to have any effect on male or female fertility in animal studies.
Use In Specific Populations
Pregnancy
Teratogenic Effects
Pregnancy Category C.
Reproduction studies have been performed in rats and rabbits. In rabbits, an incidence of 4 of 16 dams had no viable fetuses at a dose that was approximately 80 times the maximum human dose, and the highest nonembryocidal dose in rabbits was approximately 15 times the maximum human dose.
There are no adequate and well-controlled studies in pregnant women. XALATAN should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus.
Nursing Mothers
It is not known whether this drug or its metabolites are excreted in human milk. Because many drugs are excreted in human milk, caution should be exercised when XALATAN is administered to a nursing woman.
Pediatric Use
Safety and effectiveness in pediatric patients have not been established.
Geriatric Use
No overall differences in safety or effectiveness have been observed between elderly and younger patients.
Overdosage & Contraindications
OVERDOSE
Intravenous infusion of up to 3 mcg/kg in healthy volunteers produced mean plasma concentrations 200 times higher than during clinical treatment and no adverse reactions were observed. Intravenous dosages of 5.5 to 10 mcg/kg caused abdominal pain, dizziness, fatigue, hot flushes, nausea, and sweating. If overdosage with XALATAN occurs, treatment should be symptomatic.
CONTRAINDICATIONS
Known hypersensitivity to latanoprost, benzalkonium chloride, or any other ingredients in this product.
Clinical Pharmacology
Mechanism Of Action
Latanoprost is a prostanoid selective FP receptor agonist that is believed to reduce the intraocular pressure (IOP) by increasing the outflow of aqueous humor. Studies in animals and man suggest that the main mechanism of action is increased uveoscleral outflow. Elevated IOP represents a major risk factor for glaucomatous field loss. The higher the level of IOP, the greater the likelihood of optic nerve damage and visual field loss.
Pharmacodynamics
Reduction of the IOP in man starts about 3-4 hours after administration and maximum effect is reached after 8-12 hours. IOP reduction is present for at least 24 hours.
Pharmacokinetics
Absorption
Latanoprost is absorbed through the cornea where the isopropyl ester prodrug is hydrolyzed to the acid form to become biologically active.
Distribution
The distribution volume in humans is 0.16 ± 0.02 L/kg. The acid of latanoprost can be measured in aqueous humor during the first 4 hours, and in plasma only during the first hour after local administration. Studies in man indicate that the peak concentration in the aqueous humor is reached about two hours after topical administration.
Metabolism
Latanoprost, an isopropyl ester prodrug, is hydrolyzed by esterases in the cornea to the biologically active acid. The active acid of latanoprost reaching the systemic circulation is primarily metabolized by the liver to the 1,2-dinor and 1,2,3,4-tetranor metabolites via fatty acid β-oxidation.
Excretion
The elimination of the acid of latanoprost from human plasma is rapid (t½ = 17 min) after both intravenous and topical administration. Systemic clearance is approximately 7 mL/min/kg. Following hepatic β-oxidation, the metabolites are mainly eliminated via the kidneys. Approximately 88% and 98% of the administered dose are recovered in the urine after topical and intravenous dosing, respectively.
Clinical Studies
Elevated Baseline IOP
Patients with mean baseline IOP of 24 - 25 mmHg who were treated for 6 months in multi-center, randomized, controlled trials demonstrated 6 - 8 mmHg reductions in IOP. This IOP reduction with XALATAN 0.005% dosed once daily was equivalent to the effect of timolol 0.5% dosed twice daily.
Progression Of Increased Iris Pigmentation
A 3-year open-label, prospective safety study with a 2-year extension phase was conducted to evaluate the progression of increased iris pigmentation with continuous use of XALATAN once-daily as adjunctive therapy in 519 patients with open-angle glaucoma. The analysis was based on observed-cases population of the 380 patients who continued in the extension phase.
Results showed that the onset of noticeable increased iris pigmentation occurred within the first year of treatment for the majority of the patients who developed noticeable increased iris pigmentation. Patients continued to show signs of increasing iris pigmentation throughout the five years of the study. Observation of increased iris pigmentation did not affect the incidence, nature, or severity of adverse events (other than increased iris pigmentation) recorded in the study. IOP reduction was similar regardless of the development of increased iris pigmentation during the study.
Medication Guide
PATIENT INFORMATION
Potential For Pigmentation
Advise patients about the potential for increased brown pigmentation of the iris, which may be permanent. Inform patients about the possibility of eyelid skin darkening, which may be reversible after discontinuation of XALATAN [see WARNINGS AND PRECAUTIONS].
Potential For Eyelash Changes
Inform patients of the possibility of eyelash and vellus hair changes in the treated eye during treatment with XALATAN. These changes may result in a disparity between eyes in length, thickness, pigmentation, number of eyelashes or vellus hairs, and/or direction of eyelash growth. Eyelash changes are usually reversible upon discontinuation of treatment.
Handling The Container
Instruct patients to avoid allowing the tip of the dispensing container to contact the eye or surrounding structures because this could cause the tip to become contaminated by common bacteria known to cause ocular infections. Serious damage to the eye and subsequent loss of vision may result from using contaminated solutions [see WARNINGS AND PRECAUTIONS].
When To Seek Physician Advice
Advise patients that if they develop an intercurrent ocular condition (e.g., trauma or infection) or have ocular surgery, or develop any ocular reactions, particularly conjunctivitis and eyelid reactions, they should immediately seek their physician's advice concerning the continued use of the multiple-dose container.
Use With Contact Lenses
Advise patients that XALATAN contains benzalkonium chloride, which may be absorbed by contact lenses. Contact lenses should be removed prior to administration of the solution. Lenses may be reinserted 15 minutes following administration of XALATAN.
Use With Other Ophthalmic Drugs
If more than one topical ophthalmic drug is being used, the drugs should be administered at least five (5) minutes apart.
