Mohs Surgery for Skin Cancer
- What Is Mohs Surgery
- Dermatologist/Specialist
- Skin Cancer
- Preparing for Mohs Surgery
- Complications
- Recovery/Aftercare
- Cost
- Skin Cancer Treatments
What is Mohs surgery?

Mohs surgery, also referred to as Mohs micrographic surgery (MMS), is a special technique that utilizes both pathology and surgery to remove skin cancers in a physician's office. Tissue containing the tumor is frozen on a cryostat, and very thin horizontal slices of tissue are cut from the bottom-most layers of the skin tumor, positioned on a glass slide, and stained by a technician. The physician then examines these thin layers under a microscope. A dermatologist removes and examines repeated saucer-shaped layers of tissue until no more skin cancer is visible, only healthy tissue.
The procedure includes special dyes that allow the surgeon to remove the entire malignancy using a tumor map showing the sites of any residual cancer cells. During MMS there is an examination of the entire tumor's margins simultaneously while the patient is waiting. If more cancer cells are seen under the microscope, tissue is removed at those sites of involvement. Each skin layer that is removed is called a "level." If no more cancer cells are seen at a particular level, then it is deemed "clear" (no more tumor) and no additional levels are removed.
By removing only tissue where cancer is known to be present, the technique combines a very high cure rate with excellent preservation of normal skin. Once the cancer has been fully removed, the surgeon will determine the type of repair for the best cosmetic result. The surgeon may refer patients to another physician for wound closure, may close the wound immediately, or may let the wound heal on its own.
MMS is special because the entire edge and under-surface of each skin cancer layer is microscopically examined for the presence of cancer cells. Traditional surgical pathology techniques use vertical sections (bread loafing) and are only helpful to evaluate 1%-3% of the tumor margins, thereby increasing the chances that a small tumor cluster may be missed and left behind. MMS enables the examination of 100% of the entire tumor's margin, thereby reducing the chance of recurrence of the skin cancer.
MMS surgery is significantly more labor intensive than conventional methods of skin cancer treatment, and as a result, it is more expensive. This type of surgery is typically reserved only for certain situations, which include recurrent cancers that have not been cured by conventional techniques, large tumors with indistinct margins, tumors that occur in cosmetically sensitive areas like the mid-facial tissues, and scarring basal cell cancers, which are known to have a high recurrence rate.
MMS is scheduled with the understanding that the patient may be spending the entire day in the office depending on the number of levels necessary to clear the tumor. Most of these procedures are performed with the patient in the waiting room awaiting the verdict from the Mohs surgeon.
Why is the procedure called Mohs?
Mohs is named after its inventor, Dr. Frederic Mohs, who first described the technique in 1941. He originally used fixed stained tissue and patients were frequently required to spend more than one day for successful treatment. This unique technique made it possible to examine horizontal pieces of tissue from the deepest portion of the specimen while at the same time visualizing the outside edges of the tumor in the same block of tissue.
Where can I have Mohs surgery? How long does Mohs surgery take?
Mohs micrographic surgery is usually performed in an outpatient setting, such as in a doctor's office, using local anesthetic (lidocaine). Sometimes the procedure may be performed in an outpatient surgical center with the assistance of an anesthesiologist. Rarely, it is performed in an inpatient hospital setting.
You are generally in the medical office for several hours on the day of your Mohs procedure. Depending on the size and depth of the skin cancer, more than a single level may be required to achieve clearance. MMS requires your patience and your doctor's careful effort and skill. It is not always possible to predict ahead of time how many hours your specific procedure will take. Most patients leave their day's schedule open to allow for adequate time to complete their Mohs procedures.
What kind of physician can perform Mohs surgery? Where can I find a doctor board-certified in Mohs?
Most Mohs surgeons are specially trained dermatologists. There are also some plastic surgery and ear, nose, and throat (ENT) surgeons who are also trained to perform Mohs.
There is no current board certification for Mohs surgery. There are two nationally recognized MMS specialty groups, the American College of Mohs Micrographic Surgery and Cutaneous Oncology and the American Society for Mohs Surgery.
Is Mohs only for skin cancer?
Yes, Mohs is a widely used method of removing the most common types of nonmelanoma skin cancers, including basal cell carcinoma and squamous cell carcinoma. Less frequently, Mohs may also be used for other malignant tumors. In special cases, Mohs may be used to treat malignant melanoma, lentigo maligna, dermatofibrosarcoma protuberans, Merkel cell carcinoma, microcystic adnexal carcinoma, malignant trichoepithelioma, angiosarcoma, atypical fibroxanthoma, and other cancerous skin tumors.
Am I a good candidate for Mohs surgery?
You may not be a good candidate for Mohs if you are unable to tolerate local anesthesia, have extreme anxiety, have a surgical phobia, or are in very poor health.
The best treatment choice depends on various factors, including location, type of skin cancer, past treatments, and one’s overall health. Your physician can help you sort through the different options and assist in your choice. The right decision is a very personal one.
What if I have artificial joints or other health issues?
Your surgeon needs to know of any underlying medical conditions that may affect your surgery or wound healing. You would want to be certain to tell your surgeon beforehand if you have any artificial parts (implants) like knees or hips, a pacemaker or defibrillator, or need to take antibiotics before dental procedures because of a heart condition or murmur.
Your surgeon needs to know if you have had a history of staph or other skin infections in the recent past. You may be asked to wash with a special antibiotic soap or wash like chlorhexidine (Hibiclens) the night or morning before surgery to help reduce the number of bacteria on your skin.
Patients need to also advise their surgeon of any drug allergies to anesthetics like lidocaine (Xylocaine) or procaine (Novocaine). Additionally, the surgeon may need to know of any bleeding or bruising tendencies, hepatitis, HIV/AIDS, or pregnancy.
What areas are treatable by Mohs surgery?
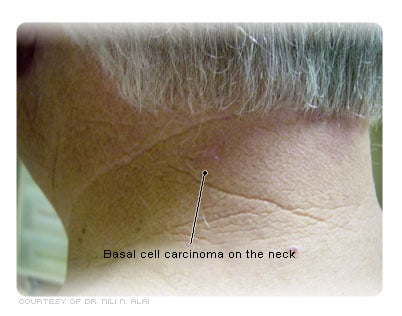
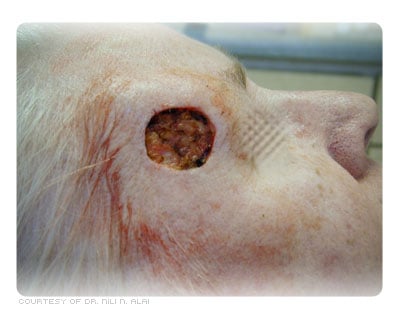
Although any skin site is amenable to MMS, it is used primarily for the treatment of head and neck basal cell carcinomas (BCCs) and squamous cell carcinomas (SCCs). It is particularly useful for skin cancers in difficult areas such as nose, lips, and ears, where it is important to remove a minimal amount of uninvolved tissue.
It is also useful on hands and feet in order to minimize scarring. MMS is very effective for the treatment of recurrent tumors (tumors that were previously removed and have regrown at the same site). However, depending on the specific patient and tumor type, any area of the body may be treated by Mohs surgery.
What are possible complications of Mohs?
As with any surgery or procedure, Mohs is associated with possible risks and complications. While it is overall a very safe and effective surgical treatment, there are some possible uncommon complications. Since a scar forms anytime you cut the skin, most patients understand and can expect some type of a scar after skin-cancer removal.
Possible risks and complications of MMS are no different from those in conventional surgical procedures and include (but are not limited to) bleeding, bruising, wound infection, pain, unsightly scar, keloid (raised, thick scar), cosmetic disfigurement, skin discoloration, nerve damage, allergic reactions, pain, reaction to local anesthesia, wound opening (dehiscence) and splitting or retained stitches, cancer recurrence, need for further surgery or treatment including radiation or plastic surgery, and very rarely death.
Minor, serious, or life-threatening side effects can occur with the use of anesthetics or with medications given before, after, or during surgery. Nerves controlling muscle movement, sensation, or other functions may be damaged. This nerve damage may be permanent. Overall, most patients tolerate the surgery very well without any complications.
What is reconstruction? Will I have a scar after Mohs surgery?
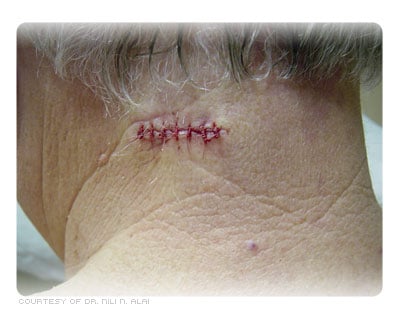
Reconstruction is repairing or fixing the wound produced after removal of the malignant skin tumor. This procedure is not different than any treatment performed after any conventional surgical procedure performed on skin. Repairing or closing the wound may involve having your surgeon stitch the wound closed side by side. Sometimes an area may heal best by letting the wound heal by itself naturally without stitches. Additional reconstruction options include using a skin graft or moving a flap of skin. Shared decision-making is very important with this issue, and it can help if you are involved by reviewing how you prefer to repair the wound.
The main goal with Mohs surgery is to remove the skin cancer in its entirety. Once the cancer is removed, then your surgeon will look at options of how to best repair the wound producing the optimum cosmetic result. The goal of MMS is to clear skin cancer, achieve the smallest scar, and preserve the maximum amount of normal tissue. Since all MMS procedures produce scars it may be necessary to consider options like lasers, scar creams and gels, and cortisone injections depending on the healing process. However, do not expect these treatments to completely remove the scar.
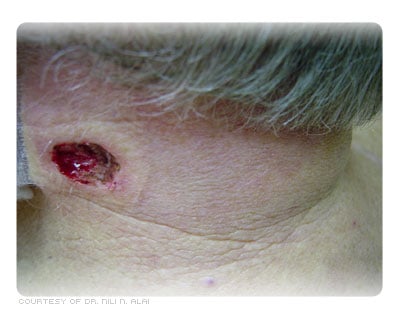
In summary, there are two parts of the procedure. The first part is the removal of the entire tumor by cutting out and examining horizontal stained frozen sections of tissue. The second portion of the procedure is the repair of the wound. Depending on a variety of factors, the wound could be reconstructed by the physician who performed the original MMS procedure, by a second surgeon (plastic or ENT), or the wound could be allowed to heal on its own (secondary intention).

What about insurance coverage and costs of Mohs surgery?
Mohs surgery is generally considered a medical service and is not considered cosmetic. Currently, most insurance plans cover the procedure under their provided benefits. However, with the many changes in insurance plans, it is always advisable to contact your insurance carrier prior to scheduling surgery and confirm your eligibility and benefits.
Mohs, like any surgical procedure, will result in additional procedure charges above the routine office-visit fees. These surgical fees may range from $1,000-$3,000 depending on the area, number of levels, and the type of closure or repair required. The greater the number of levels required, the higher the cost. Surgical centers and hospitals usually have much greater costs associated with a facility fee in addition to the surgery fee.
Insurance benefits vary and reimbursement depends on what benefits you have contracted for with your company. Currently, Medicare generally covers 80% of Mohs cancer surgery. If you have a secondary insurance plan, that may help take care of the remainder 20% not covered by Medicare.
Commercial or non-Medicare insurance generally cover a large percentage of the surgical cost, not including any deductible expense.
What are alternatives for Mohs surgery?
It is important to understand that there are alternative treatments and options to Mohs. Additional treatment choices include (but are not limited to) local radiation, plastic surgery, curettage and desiccation (scrape and burn), regular excisional surgery, cryosurgery (deep freezing), and photodynamic therapy (uses a type of light and a light-activated chemical called a photosensitizer).
How do I prepare for my Mohs surgery?
Your personal physician will give you the preoperative instructions specific for your condition.
Smoking is discouraged for at least one to two weeks before surgery. Smoking can slow wound healing and cause more wound infections.
Heavy alcohol use is not advised at least one week before surgery. Heavy alcohol use can cause more bleeding and thin your blood. An occasional glass of wine or small cocktail may not cause severe bleeding. Your physician will want to know of any factors that may affect your surgery or wound healing.
Since the duration of the procedure is not known, most patients are advised to eat a good breakfast on the day of surgery and take all of their regular daily medications. Patients are advised to wear comfortable casual clothes and bring a sweater or small blanket. In most cases, patients are able to drive after most procedures and do not necessarily need a driver unless they feel uncomfortable. Diabetic patients may need to be more cautious about maintaining good blood sugars and avoiding dangerous lows in their sugars from fasting. Bring some personal snacks, drinks, and reading or knitting material. Personal music headsets or iPods may also provide relaxation and help pass time.
For surgery center or hospital-based procedures requiring any type of sedation or general anesthesia, patients may be required to not eat or drink anything past midnight the night before surgery. Your surgeon or anesthesiologist will advise you of specific instructions before surgery.
Most patients continue all doctor prescribed medications including aspirin and any blood-thinning medication unless specifically advised otherwise only by the primary physician or plastic or Mohs surgeon. Patients with a significant history of stroke, heart attacks, or even heart pain (angina) under a doctor's care must discuss their medications with their doctor before making any changes. It is important to not discontinue blood thinners without a doctor's specific instructions because of a potential greater risk of a heart attack and/or stroke.
For otherwise healthy individuals (non-cardiac and non-stroke patients), nonessential, nonmedically prescribed medications that thin the blood -- such as ibuprofen (Advil, Motrin), aspirin, vitamin E, garlic supplements, Alka-Seltzer, Pepto-Bismol, other aspirin-containing medications, etc. -- can be stopped at least seven to 14 days before undergoing Mohs surgery to minimize bleeding and bruising. These medications can thin your blood and make you more prone to bleed during and after surgery. Again, it is important to not discontinue or start any medication without a doctor's specific instruction.
What is the recovery time for Mohs surgery? Is Mohs painful?
Recovery is usually very easy and uneventful. Overall, resting as much as possible the first few days after surgery is helpful.
Stitches (sutures) are usually removed at the surgeon's office anywhere from four to 14 days from the date of surgery. Your physician will let you know what date to return for stitch removal.
Most patients report minimal discomfort after surgery and require minimal or no pain medication.
If there is pain, many patients find that they prefer to take something for pain at the first hint of discomfort instead of waiting until the pain builds up to an unbearable level. If you have mild or moderate pain, your doctor may advise you to take acetaminophen (Tylenol) or another pain reliever over the counter. Aspirin or aspirin-containing pain relievers may cause increased bleeding. Rarely, prescription pain medications may be required for severe pain.
Your physician will let you know what pain medications are recommended for your specific condition.
Most patients are able to return to work or school the next day after Mohs. Avoiding heavy lifting, straining, or strenuous exercise for seven to 21 days may be required depending on the area of surgery. Your physician will need to let you know what activity precautions are required based on the area and size of your procedure.
You may go out in the sun with sunscreen and protective hats and clothing. Excess sun exposure has been linked to skin cancer. Use of sunscreen or other cover-up on the scar is very helpful for at least six months after surgery to help minimize scarring. It is important to follow your own physician's instructions for wound care and sun protection.
How do I take care of my surgical area after Mohs surgery?
It is recommended to check with your surgeon for specific postoperative wound care instructions. Often, you will be asked to go home and take it easy for the rest of the day. A few patients like to return to work and resume their work the day after surgery. It may be advisable to avoid heavy lifting and exercise, especially the first 24-48 hours after surgery. Your physician will usually give you more detailed instructions depending on the area and size of the surgery. You will have usually have a bulky "pressure" dressing on the surgery area for one day. You may be asked to keep the area dry for 24 hours. Swimming pools, oceans, and Jacuzzis are usually not permitted while the stitches are in. These may increase your chance of infection. Many physicians allow you to shower the next day after surgery. Wound care may require cleaning the wound with soap or hydrogen peroxide two to three times a day and applying petroleum jelly to the area. Mild swelling is not uncommon the first day or two after surgery and can be lessened by use of an ice-bag application, ice cubes or chips in a small Ziploc baggie, or frozen peas in the bag. Leaving the dressing in place, use cold pack application every five to 15 minutes every hour for the first eight to 24 hours after surgery. Swelling is more common for surgeries around the eyes or lips. Sleeping propped up on a few pillows or in a reclining chair may help decrease swelling after surgery of the head and face area.
The surgical area may ooze a little blood or clear liquid especially in the first few hours after surgery; activity may aggravate this. Hot drinks or bending over at the waist can also initiate or worsen bleeding of face wounds. If bleeding occurs, firm pressure applied directly to the site for 10-15 minutes may be helpful. Most bleeding will stop if you apply enough pressure. Your surgeon should be notified if bleeding persists. Rarely, a visit to the hospital emergency room may be necessary for severe bleeding.
Your surgeon will need to know if pain is increasing after one to two days after your surgery or if you are having fever or other concerning symptoms. In such cases, you may need to be seen at the surgeon's office. The surgical area may need to be checked for bleeding or infection. Limiting hot foods, hot drinks, and heavy chewing for 48 hours may help decrease the chances of postoperative bleeding for wounds around the mouth or cheek areas. Your physician will explain recommended wound care.
Most patients are advised to try to avoid applying makeup or powder directly on a fresh wound unless the surface is fully healed. Skin-colored tape strips called Steri Strips are available to minimize wound leakage and help cover up a visible wound. It is important to follow your physician's instructions for wound care.
What is the chance that my cancer will recur after Mohs surgery?
There is a very low chance that your skin cancer will recur after Mohs surgery. Cure rates have been reported as high as 96%-99%.
It is important to understand that no cancer treatment or surgery has a 100% cure rate. A skin cancer may recur or a new cancer may arise in the same or adjacent area even after Mohs or other surgery. Some skin cancers are more aggressive than others and need additional treatment and closer follow-up. Skin cancers frequently need additional follow-up and possible further treatment. Although MMS surgery tends to have the highest cure rate compared to other treatments, it may need to be supplemented by radiation or further surgery. Follow-up appointments with your physician are very important, especially in the first few years after surgery. Many patients are seen every four to six months after their diagnosis of a skin cancer. Monthly self-examinations of the skin are good practice for patients with a history of skin cancer. Any changing or new growth should be promptly checked by your physician. More regular follow-up appointments may be needed for those with more aggressive tumors or tumors in high-risk areas.
How many "levels" of Mohs surgery will I need?
On average, most patients may only need one or two levels before clearing the tumor. Depending on the skin cancer type and location, a patient may need anywhere from one to 10 or more levels to clear a tumor.
There is very little way to predict beforehand how large a skin cancer is because often there are invisible portions that can be seen only with the help of a microscope. Sometimes, more than one surgical procedure may be required to remove very large or invasive tumors, cancers in small areas or difficult areas, or to obtain the best medical and cosmetic result.
What are treatment options for skin cancers?
There are many effective ways to treat skin cancers. Options include local radiation (X-ray) treatments, curettage and desiccation "C&D" (scrape and burn), cryosurgery (specialized deep freezing), photodynamic therapy using Levulan and laser and or blue light, regular surgical excision, laser removal and surgery, Mohs surgery, and several prescription creams, including imiquimod (Aldara) and fluorouracil (Efudex).
