Achilles Reflex
Clinical Examination Technique
The Achilles reflex (or ankle jerk reflex) is elicited by a rapid stretch of the Achilles tendon. The examiner strikes the tendon with a reflex hammer, which should cause a contraction of the gastrocnemius and soleus muscles, resulting in plantar flexion of the foot at the ankle.
For best results, the patient should be relaxed. The reflex can be tested with the patient seated with their knee bent and foot dangling, or kneeling on a chair. Gentle dorsiflexion of the foot by the examiner before striking the tendon can enhance the response.
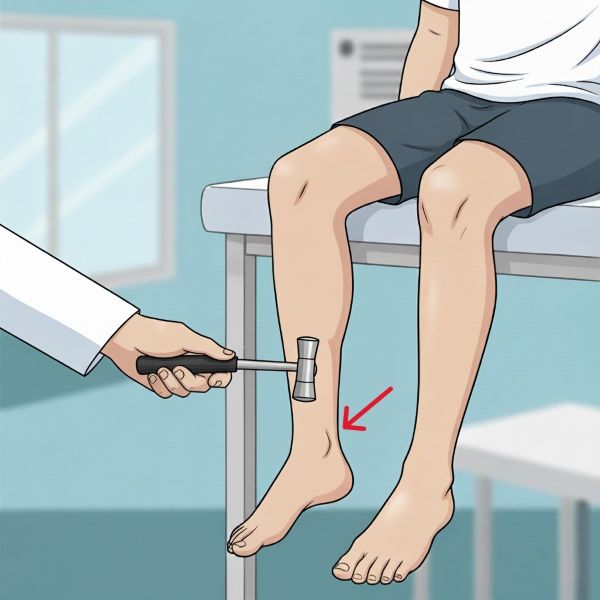
Eliciting the Achilles reflex. The foot is gently dorsiflexed to put tension on the tendon before it is struck with a hammer.
Neural Pathway
The Achilles reflex is a deep tendon reflex mediated primarily through the sacral spinal segments S1 and S2. The afferent (sensory) and efferent (motor) signals are carried by the sciatic nerve and its continuation, the posterior tibial nerve.
Clinical Significance
The status of the Achilles reflex is a valuable diagnostic clue:
- Absent or Diminished (Hyporeflexia): A lost reflex is a key sign of a lower motor neuron lesion. It is a common finding in peripheral polyneuropathies (e.g., diabetic neuropathy), S1 radiculopathy (e.g., from a herniated disc), and can also be diminished or absent as a consequence of normal ageing.
- Brisk (Hyperreflexia): An exaggerated reflex is a sign of an upper motor neuron lesion, suggesting pathology in the spinal cord or brain that is interrupting descending inhibitory signals.
- Slow-Relaxing: A visibly slow relaxation phase of the reflex (Woltman sign) is a classic sign of hypothyroidism.
Cross References
Age-related signs; Neuropathy; Reflexes
